Influenza Virus (About the EoE)
Contents
- 1 Influenza Virus
- 2 1918 Spanish Flu
- 3 Discovery of the Influenza Virus
- 4 Structure of the Influenza Virus
- 5 How the Influenza Virus Replicates and Spreads
- 6 How to Stop the Spread of the Influenza Virus
- 7 How is the Influenza Virus Outmaneuvering Us?
- 8 Are Humans Worsening the Problem?
- 9 Steps to Protect Yourself Against the Flu Virus
- 10 References and Further Reading
Influenza Virus
| Topics: |
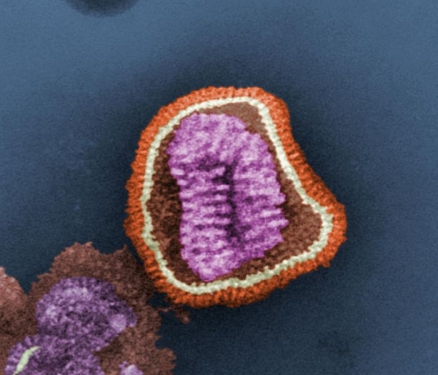
This (Pseudocolored) negative-stained (false-colored) transmission electron micrograph (TEM) depicts the ultrastructural details of an influenza virus particle, or “virion”. (By Photo Credit: Cynthia Goldsmith Content Providers(s): CDC/ Dr. Erskine. L. Palmer; Dr. M. L. Martin Domain, via Wikimedia Commons)
Though the influenza virus has been killing humans for thousands of years, the virus itself was not discovered until the 1930s. Without the knowledge about the origin and transmission of this disease, the 1918 Spanish flu had a terrible impact, infecting about 30%,and killing about 3%, of the world’s population. To develop vaccines and drugs against viruses, researchers target specific viral components involved in viral entry and viral budding. But with their high mutation rates and ability to evolve rapidly, viruses have the upper hand in the co-evolutionary race against humans. If the 2003 Severe Acute Respiratory Syndrome (SARS) outbreak is any indication, the next global pandemic (disease spread over a large region) is on its way, and the worst may be yet to come. The question asked every year then, by experts and the common person alike, is when will it strike and will the world be prepared?
 Gym full of victims of the 1918 Spanish Flu outbreak. Source: Dartmouth Medicine Magazine
Gym full of victims of the 1918 Spanish Flu outbreak. Source: Dartmouth Medicine Magazine
1918 Spanish Flu
How would the world today respond to an infectious disease spread worldwide, one that took more American lives than World Wars 1 &2, the Korean War, and the Vietnam War combined? It is not just the number of deaths that is striking. Typical cases of influenza target the youth and elderly populations. But, the 1918 pandemic was unique in that healthy individuals in the 15-40 age group endured the highest death rates. Within days, patients could progress from a high fever to suffering from fluid accumulation in the lungs, skin discoloration, and loss of blood from the nose. At the time, doctors thought bacteria were the culprits because the influenza virus had yet to be discovered. Even though the world did not have the technological means to stop the virus at the time, the viral Spanish flu disappeared on its own later in the year. However, the viral strain disappeared only after taking the lives of about 50 million people worldwide, including approximately 675,000 Americans. Another 20 million Americans fell ill.
Discovery of the Influenza Virus
The high death rates caused by the 1918 Spanish flu are not surprising. First off, physicians did not have effective influenza drugs or vaccines. In addition, not knowing how influenza spreads prevented them from taking appropriate measures to reduce the transmission rate. Though humans likely were first infected with influenza virus thousands of years ago when they began to domesticate animals, it was not until 1933 that the human influenza virus was first isolated and associated with the disease.
Wilson Smith infected ferrets with mucus from a human infected by the flu virus. As Smith observed the sick ferrets, one of the ferrets sneezed in his face, transferring the flu to him. When Smith examined the viral strain infecting his throat, he discovered that the strain was the same one that the ferret had. Through this study, he showed that the flu virus could be transferred from one animal to another animal and also from an animal to a human. Next, Smith and his team discovered that ferrets exposed to a sample of the influenza virus were protected from the virus when they were later infected with the same strain. This knowledge, along with understanding the structure of the virus, was fundamental to developing the first vaccines.
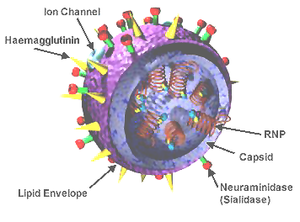 Influenza virus structure. Source: California Department of Health Services.
Influenza virus structure. Source: California Department of Health Services.
Structure of the Influenza Virus
Before vaccines could be developed against the influenza virus, researchers first studied its structure.
The influenza virus that infects humans has a single stranded RNA genome made of eight genes that code for eleven proteins. Three of these proteins are RNA polymerases, which are necessary for influenza to replicate its RNA genome in animals and humans.
The viral genome is surrounded by a capsid that is made up of capsid nucleoproteins (NP), nonstructural protein 1 (NS1), and Nuclear Export Protein (NEP). The NEP protein is involved in the regulation of viral transcription and genome regulation, both which contribute to the pathogenicity of the virus. The capsid is surrounded by a lipid envelope, which contains M2 proteins that form ion channels to control pH of the viral envelope. In addition, the envelope contains the neuraminidase (NA) antigen and the hemagglutinin (HA) glycoprotein, which the virus uses to recognize sialic acid receptors on the host cell membrane.
The type of influenza of concern for the general public is Type A Influenza. This type of influenza can infect both people and animals, with wild birds commonly serving as the host. The different Type A strains are named for the NA and HA surface glycoproteins found on the viral envelope. Thus, the viral strain that caused the 2003 SARS outbreak, the H1N1 virus, was named for displaying the HA 1 protein and NA 1 protein. Types B and C are much less pathogenic to humans.
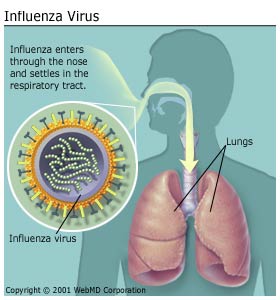 Influenza virus transmission via air. Source: Web MD.
Influenza virus transmission via air. Source: Web MD.
How the Influenza Virus Replicates and Spreads
The flu virus spreads quickly in crowded areas since it spreads through human populations via air and also through contact with infected surfaces such as doorknobs and water fountains. An infection can start in a person’s upper respiratory tract when a person breathes in aerosols containing the influenza virus from another infected individual. Once the influenza virus enters the person’s respiratory tract, the HA glycoprotein will bind to a receptor on the host cell. As the glycoprotein is split by a host cell protease, the capsid of the virus is released into the host cell and after an uncoating process, the genome is replicated to produce the RNA and translated to produce the capsid proteins needed. Then, after a spontaneous self-assembly process, the newly produced influenza virus can leave the host and spread to other individuals.
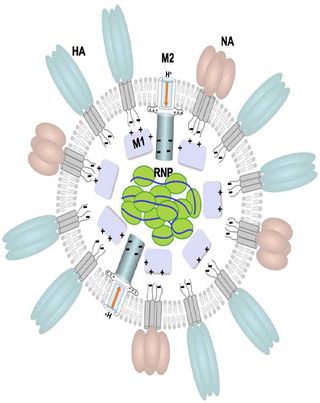 Viral drug targets. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3108042
Viral drug targets. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3108042
How to Stop the Spread of the Influenza Virus
To design effective antiviral drugs, researchers target components of viruses that are not found in human cells. The M2 protein that forms the proton channels of the viral envelope is needed to maintain the pH required for successful viral entry into the host cell. Early antiviral drugs, such as Amantadine and Rimantadine, kept this channel closed, hindering the entry of influenza viruses into host cells. As mentioned earlier, NA and HA glycoproteins are found on the viral envelope. The HA glycoprotein allows the virus to recognize the host cell receptor; the NA cell surface glycoprotein allows the virus to leave the cell via budding to infect another cell. To prevent viruses from spreading, NA inhibitors such as Oseltamivir, more commonly known as Tamiflu, will block the budding process of viruses. With drugs that can target specific structures, how are humans losing the war against viruses?
How is the Influenza Virus Outmaneuvering Us?
Humans and the flu virus are locked in a co-evolutionary race. Viruses have been able to be become resistant to drugs and vaccines due to characteristics that contribute to high evolutionary rates, which include large population sizes and very short generation times. In addition, viral replication machinery (RNA polymerases) does not have proofreading capability, leading to high error rates. Thus, viruses can quickly accumulate mutations. Gradually, mutations can accumulate in the genes that code for the viral NA and HA antigens, causing a process called antigenic drift. Another way in which viruses can evolve is called antigenic shift. This process occurs when two or more virus strains infect the same host cell. When new viruses are ready to self-assemble, proteins from different viral strains may accidentally become packaged within one virus. Thus, a completely new viral subtype featuring a mixture of surface antigens is produced. Since antibodies target specific antigens, the immune system may no longer recognize the specific antigen, not being able to mount a quick and powerful response against the virus. Thus researchers are in a constant battle with viruses every flu season as they try to create new vaccines to respond to antigenic drift and shift.
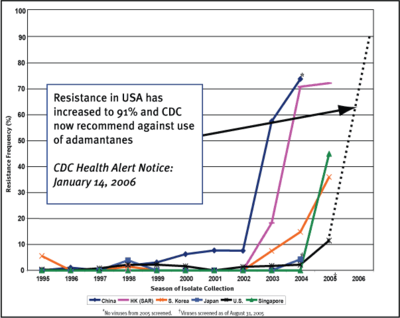 Viral resistance to the drug Amantadine. Source: Qiagen.
Viral resistance to the drug Amantadine. Source: Qiagen.
Are Humans Worsening the Problem?
Yes. Humans are aiding viruses by misusing antiviral drugs. In China, farmers try to reduce the outbreak of the bird flu among chickens by using the antiviral drug Amantadine, injecting it directly into the animals or including it in the drinking water of chickens. The misuse of this drug, originally meant for humans, is selecting for more resistant strains of influenza virus.
But, as explained earlier, humans are not entirely to blame for the phenomenon of viral resistance. Viruses are better equipped to adapt to their environment due to their short generation times, large populations, and high mutation rates. Viral resistance to the anti-viral drug Amantadine has skyrocketed, as shown in the figure, just within a nine-year span from 1995 to 2006. It is not surprising then that in 2004, Vietnam had to use an alternative, more expensive drug since the H5N1 flu strain had become resistant to Amantadine.
With some strains of influenza already highly resistant to the antiviral drugs Amantadine and Rimantadine, and new strains developing resistance to a third drug Tamiflu, researchers have been testing a combination of the three to combat the rapidly mutating influenza virus. Adamas Pharmaceuticals is a private company that has already shown in animal trials that this triple therapy is more effective than the use of two or just one drug. The triple therapy is currently in human clinical trials in North America with results expected in September 2014.
What are the Symptoms of the Flu?
Influenza is a contagious respiratory illness that can result in symptoms ranging from mild to deadly. Unlike the common cold, the flu usually often appears without warning. Symptoms include: diarrhea and vomiting (more common in kids than adults), fatigue, fever, headaches, running nose, and sore throat. Though most people recover from the flu within a few days without antiviral drugs, others can develop more serious forms that require medical attention. It is not uncommon to develop bronchitis, pneumonia, and ear infections from the flu as a result of having a weakened immune system.
Steps to Protect Yourself Against the Flu Virus
The Centers for Disease Control and Prevention (CDC) recommends that the general public follow three major steps to protect themselves and their families. The first is to take a yearly flu vaccine. The seasonal flu vaccine is designed to protect against the three most common viral strains. Those older than six months of age are advised to take a flu vaccine, especially if they are around children younger than six months of age, who are too young to be vaccinated. Which subsets of the general public are most at risk from developing a serious form of the flu virus? Children under the age of five (especially those under the age of two), adults over the age of 65, pregnant women, and those with chronic conditions such as asthma (Asthma Triggers), heart disease, and compromised immune systems (such as patients with cancer and AIDS).
The second step relies on taking everyday precautions. Covering your nose and mouth when you sneeze, disinfecting surfaces, and not touching your eyes, nose, and mouth can help slow the spread of pathogens.
When you do fall ill to the flu, it is important to stay out of the public for at least 24 hours even after your fever disappears. If it is serious and requires medical attention, make sure that you take antiviral drugs and not antibiotics. Taking antibiotics, which treat bacterial infections, worsen the problem of antibiotic resistance, a problem as serious as viral resistance.
References and Further Reading
- Centers for Disease Control and Prevention, (2011). Influenza (flu) viruses
- Conner, S. (2013, May 2). Appalling irresponsibility: Senior scientists attack chinese researchers for creating new strains of influenza virus in veterinary laboratory. The Independent
- *Lambert, L., & Fauci, A. (2010). Influenza vaccines for the future. The New England Journal of Medicine, 363, 2036-2044.
- Taubenberger, J. (2010). Influenza: The once and future pandemic. Public Health Reports, 125(3), 16-26.
- Top 10 questions about the flu. (2011, September 21). Retrieved from http://editors.eol.org/eoearth/wiki/Influenza_Virus_(About_the_EoE)