Haiti Cholera Outbreak (FAQ)
Contents
- 1 Frequently Asked Questions About the Haiti Cholera Outbreak
- 1.1 When was cholera first detected in Haiti?
- 1.2 How long will the cholera outbreak in Haiti last?
- 1.3 Is the current outbreak a result of the January 2010 earthquake in Haiti?
- 1.4 What is cholera?
- 1.5 What are the symptoms of cholera?
- 1.6 How does a person get cholera?
- 1.7 Can cholera be spread from person to person?
- 1.8 How is cholera treated?
- 1.9 Where can cholera be found?
- 1.10 How can cholera be prevented?
- 1.11 Citation
Frequently Asked Questions About the
Haiti Cholera Outbreak
When was cholera first detected in Haiti?
The outbreak of cholera was confirmed in Haiti on October 21, 2010.
How long will the cholera outbreak in Haiti last?
Although we can’t be certain, experience from the Peru outbreak in the early 1990s and from other countries in Latin America suggests that we should expect to identify additional cases for many months to several years.
Is the current outbreak a result of the January 2010 earthquake in Haiti?
No, the current outbreak is not a result of the January 2010 earthquake. Outbreaks of epidemic cholera have not been documented in Haiti before or anywhere in the Caribbean since the mid-nineteenth century. For a cholera outbreak to occur, two conditions have to be met: (1) there must be significant breaches in the water, sanitation, and hygiene infrastructure used by groups of people, permitting large-scale exposure to food or water contaminated with Vibrio cholerae organisms; and (2) cholera must be present in the population. While it is unclear how cholera was introduced to Haiti, both of these conditions now exist.
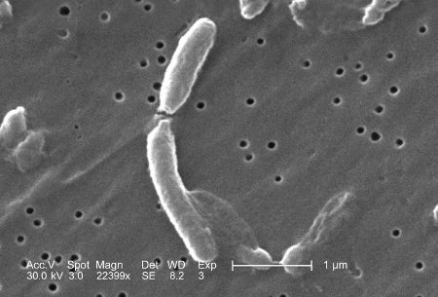
What is cholera?
Cholera is an acute, diarrheal illness caused by infection of the intestine with the bacterium Vibrio cholerae. The infection is often mild or without symptoms, but sometimes it can be severe.
What are the symptoms of cholera?
Cholera infection is often mild or without symptoms, but can sometimes be severe. In severe cases, the infected person may experience profuse watery diarrhea, vomiting, and leg cramps, which can cause rapid loss of body fluids and lead to dehydration and shock. Without treatment, death can occur within hours.
How does a person get cholera?
A person can get cholera by drinking water or eating food contaminated with the cholera bacterium. In an epidemic, the source of the contamination is usually the feces of an infected person that contaminates the food and/or water. The disease can rapidly spread in areas with inadequate treatment of sewage and drinking water, such as Haiti. However, at this time the origin of this outbreak is unknown and CDC hopes to learn more in the course of its response to this outbreak.
Can cholera be spread from person to person?
Person-to-person transmission is extremely rare, even to healthcare workers during epidemics. Drinking water and food contaminated with Vibrio cholerae from the feces of an infected person is the most common source of cholera infections.
How is cholera treated?
Cholera can be treated by immediately replacing fluids and salts lost through diarrhea using oral rehydration solution. This solution is used throughout the world to treat diarrhea. Antibiotics may also be used to shorten the course and diminish the severity of the illness. However, they are not as important as receiving oral or intravenous rehydration therapy.
Where can cholera be found?
Cholera is found naturally in the environment in many areas around the world and can move from place to place via contaminated water or food, or infected people.
How can cholera be prevented?
Cholera can be prevented by both visitors and residents of Haiti by following the Five Basic Cholera Prevention Messages:
- Drink and use safe water*
- Bottled water with unbroken seals and canned/bottled carbonated beverages are safe to drink and use
- Use safe water to brush your teeth, wash and prepare food, and to make ice
- Clean food preparation areas and kitchenware with soap and safe water and let dry completely before reuse*Piped water sources, drinks sold in cups or bags, or ice may not be safe and should be boiled or treated with chlorine.
To be sure water is safe to drink and use: - Boil it or treat it with a chlorine product or household bleach
- If boiling, bring your water to a complete boil for at least 1 minute
- To treat your water with chlorine, use one of the locally available treatment products and follow the instructions
- If a chlorine treatment product is not available, you can treat your water with household bleach. Add 8 drops of household bleach for every 1 gallon of water (or 2 drops of household bleach for every 1 liter of water) and wait 30 minutes before drinking
- Always store your treated water in a clean, covered container
- Wash your hands often with soap and safe water*
- Before you eat or prepare food
- Before feeding your children
- After using the latrine or toilet
- After cleaning your child’s bottom
- After taking care of someone ill with diarrhea* If no soap is available, scrub hands often with ash or sand and rinse with safe water.
- Use latrines or bury your feces (poop); do not defecate in any body of water
- Use latrines or other sanitation systems, like chemical toilets, to dispose of feces
- Wash hands with soap and safe water after defecating
- Clean latrines and surfaces contaminated with feces using a solution of 1 part household bleach to 9 parts waterWhat if I don’t have a latrine or chemical toilet?
- Defecate at least 30 meters away from any body of water and then bury your feces
- Dispose of plastic bags containing feces in latrines, at collection points if available, or bury it in the ground. Do not put plastic bags in chemical toilets
- Dig new latrines or temporary pit toilets at least a half-meter deep and at least 30 meters away from any body of water
- Cook food well (especially seafood), keep it covered, eat it hot, and peel fruits and vegetables*
- Boil it, Cook it, Peel it, or Leave it
- Be sure to cook shellfish (like crabs and crayfish) until they are very hot all the way through*Avoid raw foods other than fruits and vegetables you have peeled yourself.
- Clean up safely—in the kitchen and in places where the family bathes and washes clothes
- Wash yourself, your children, diapers, and clothes, 30 meters away from drinking water sources
What is the risk for cholera in the United States?
In the United States, cholera was prevalent in the 1800s but water-related spread has been eliminated by modern water and sewage treatment systems. However, U.S. travelers to areas with epidemic cholera (for example, parts of Africa, Asia, or Latin America) may be exposed to the cholera bacterium. Additionally, travelers may bring contaminated seafood back to the United States, which can result in foodborne outbreaks of cholera.
Does CDC recommend cholera vaccines for people traveling to Haiti?
At this time, CDC does not recommend cholera vaccines for travelers since their risk of contracting the disease is extremely low. For cholera vaccine to be effective, people need two doses, and it takes time for vaccinated people to become immune. Multiple weeks can elapse before they are protected following vaccination. Since most people travel for a short period of time, the vaccine is not recommended. Basic hygiene precautions should always be taken.
Where can travelers get information about cholera?
Information can be accessed on CDC’s Travelers’ Health Website as well as the CDC Cholera Website.
What is CDC doing to combat the current cholera outbreak in Haiti?
CDC, in collaboration with the US government led by USAID, is assisting the government of Haiti, PAHO and several other international health agencies in responding to the cholera outbreak. There are several laboratory tests in progress in CDC labs, including a variety of molecular tests, which will help determine the genetic connections between the bacterial isolates from the Haiti outbreak and other strains around the world. CDC will continue to gather information about outbreak strains for comparison to other known cholera strains. However, the most important goals right now are to save lives and reduce the spread of disease in Haiti.
Editor's Note
- November 7, 2010, 12:30 AM ET